‘It’s like working in a disaster zone’; Long-term care workers in eye of COVID-19 storm
Posted: April 4, 2020
(April 3, 2020)
By: Pj Wilson, North Bay Nugget
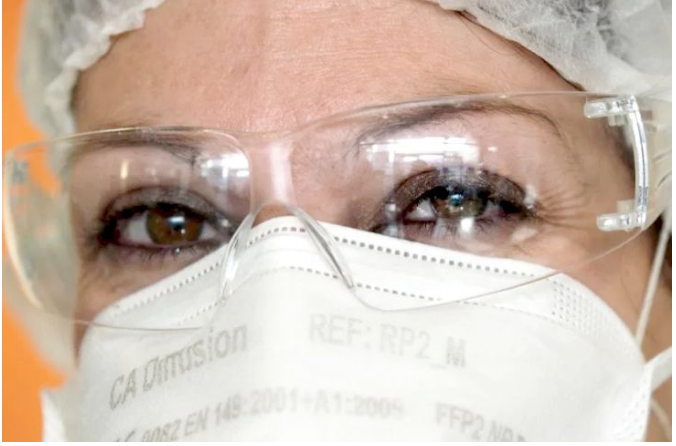
N95 masks are not being made available to all long-term care workers because of a shortage of personal protective equipment, says Candace Rennick, secretary-treasurer of the Canadian Union of Public Employees in Ontario. Getty Images.
Health-care workers are operating in “war-zone conditions” because of the outbreak of COVID-19 around the world.
Candace Rennick, secretary-treasurer of the Canadian Union of Public Employees in Ontario, says a shortage of personal protective gear – PPE – leaves long-term care employees ill-prepared to deal with the pandemic.
“It’s like working in a disaster zone,” Rennick says. “There is a lot of fear.”
What makes things worse, she says, is the province “loosened up a whole bunch of rules” to bring in volunteers at many of the facilities, although many are not trained and have no experience dealing with infectious diseases.
“It’s a perfect storm that is leading to disaster,” she says.
“It’s only going to get worse.” One of the first things Rennick would do is have every longterm care facility – and in fact, any health-care facility – treat COVID-19 as though it is an airbone-transmissible disease.
During the SARS crisis in 2003, she says, the initial belief was that it could not be transmitted through the air. It was later determined that it could. In that crisis, 375 Canadians were infected and 44 died.
As of Wednesday, 9,560 Canadians had contracted COVID-19 and 112 died.
Workers, Rennick says, should have access to “proper full protective equipment,” including N95 masks, which are used to protect the wearer from airborne particles and from liquid contaminating the face.
“But they are not being made available,” Rennick says. “We don’t have an adequate supply.”
Long-term care patients, she says, are the most vulnerable to contracting the virus, and if it gets into a facility is “able to spread like wildfire.
Despite the efforts of long-term care administration, “staff are fearful,” says Amanda Farrow, president of CUPE Local 1339.
“I would like to think management is doing the best they can,” she says, but the protocols put in place by the province set only minimum standards.
“The homes are doing what they are directed to do by the ministry” of long-term care, she says. “That doesn’t alleviate the fears of the workers.
“The information is changing all the time. We don’t know what tomorrow will bring.
“People are afraid. I don’t think anyone walks in the door and says “I’m immune.'” Over the past few days, Farrow says, staff at Eastholme Home for the Aged have been required to wear surgical masks all the time when they are on the unit.
“It elevates the fear for sure,” she says.
“This is what everyone is talking about.”

Olive Street residents make their thoughts known with a large sign set up in front of their home, Wednesday. PJ Wilson/The Nugget
And while the information is constantly changing, Farrow says administration at Eastholme is “trying to communicate the most up-to-date information” to staff.
What needs to happen, though, is for the province to do a better job of elevating the minimum standards, as well as providing all employees with PPE.
Fourteen residents and one volunteer at the Pinecrest Nursing Home in Bobcaygeon have died of the virus, and there have been 19 other COVID-19-related deaths at long-term care and retirement homes in the province.
Many staff at the Bobcaygeon facility tested positive and were placed in mandatory isolation.In a release issued Tuesday, the Ontario Health Coalition said Ontario trails all provinces in testing for coronavirus, with only 334 per 100,000 people being swabbed.
Alberta is testing three times as many residents, while five times as many are being tested in the Northwest Territories.”The (Doug) Ford government has said that the reason is a lack of reagents needed for testing,” the coalition notes. “But Ontario not only lags in the number of tests per capita (which one might expect given the size of the population), our province has also done fewer tests in total than our nearest large province and is very close in total numbers to other large provinces that have much smaller populations. Which raises the question – if other provinces have enough reagents to do more tests, then why does Ontario not?”The national labour union CLAC also sounded the alarm on Tuesday, warning nursing homes will become vectors for COVID-19 unless more protective equipment is immediately supplied.”Recent outbreaks in two Ontario longterm care homes demonstrate that COVID-19 is clearly spreading in ways that current policies are failing to address, and that includes failing to protect people from airborne droplets arising from regular or heavier breathing,” said Michael Reid, CLAC’s Ontario health-care coordinator.The organization is calling on the Ford government to both boost PPE and implement stronger usage protocols in longterm care homes to protect frontline workers and residents.
Click here for original article


