REPORT: Tracking of COVID-19 Outbreaks in Health Care Settings – Data Updated to June 2
Posted: June 5, 2020
(June 5, 2020)
——-
Introduction
Each number included in this tracking data represents a human being who is loved and who has experienced the terrible toll of COVID-19: staff who have gone to work despite the risk and the fear; residents and patients who have contracted COVID-19; families and communities who have lost their loved ones; staff who have made the ultimate sacrifice. You are in our hearts. To the media, the Public Health and Ministry staff who have been tracking and compiling this information for public scrutiny, thank you for your work. To all of you, we give our commitment to advocate to the best of our ability and to do everything we can do for the best protection and care for all affected.
This report is the result of many hours of work by our staff and volunteers.
A special thank you is due to the following volunteers who have gone above and beyond to help track the spread of COVID-19 in health care settings in their communities:
Nick Alpin, Rose Anderson, Roy Brady, Rolf Gerstenberger, Matthew Gventer, Sue Hotte, Dot Klein, Claire Lownie, Mary Catherine McCarthy, Magee McGuire, Tracey Ramsey, Shirley Roebuck, Mervyn Russell, Stuart Ryan, Samrin Sobahan, Bryan J. Smith, Jim Stewart, Jules Tupker
A special and heartfelt thank you also to Megan Lee, Riley Sanders and Salah Shadir, our intrepid and talented staff who have worked day and night to research, fact check and distribute these tracking report updates throughout the pandemic.
We are deeply grateful and we simply could not have continued to do this work without all of you. Thank you.
Natalie Mehra, Executive Director
Summary & Charts
Since the week of March 12, the Ontario Health Coalition has been tracking all people who have been infected with COVID-19 in outbreaks in health care settings including hospitals, long-term care, retirement homes, public health units, clinics and congregate care settings, as well as among other health professionals such as paramedics. This has become a gargantuan task but an important one because it enables us to see more fully than is possible from the government data where the spread in health care is happening and whether infection control measures are working to control it. The evidence shows that by every measure the outbreaks in health care settings are not under control and that more effective measures are needed to protect residents, patients and staff. While the number of facilities in outbreak has stabilized, the numbers of residents/patients and staff infected in outbreaks and, tragically, dying, are still growing at a significant rate. On a positive note, the rate of growth though it is still dramatic, has decreased from its highest rate (April 21 – May 5) since the beginning of the pandemic when the first outbreaks were discovered, testing began, and there was a sudden increase.
Here are the key findings from the most recent tracking contained in this report of cases in health care settings across Ontario up to the afternoon of June 2:
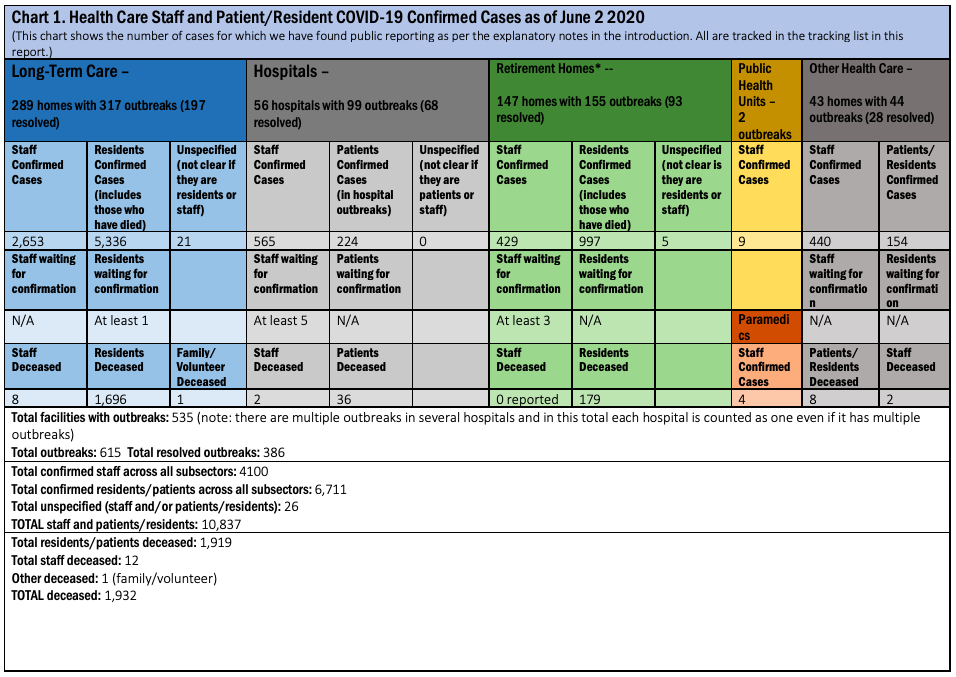
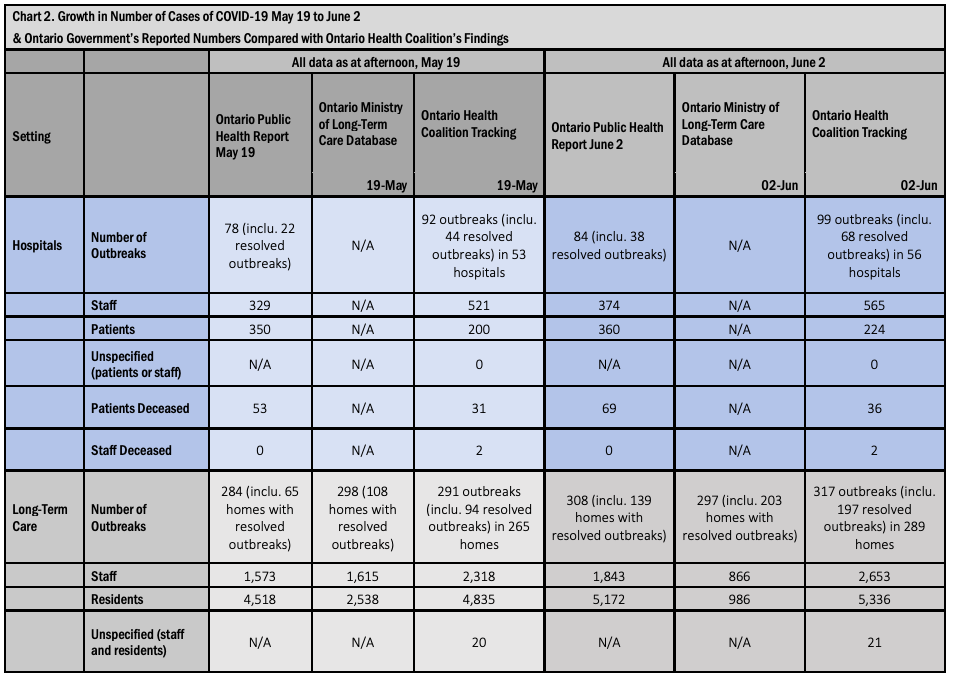
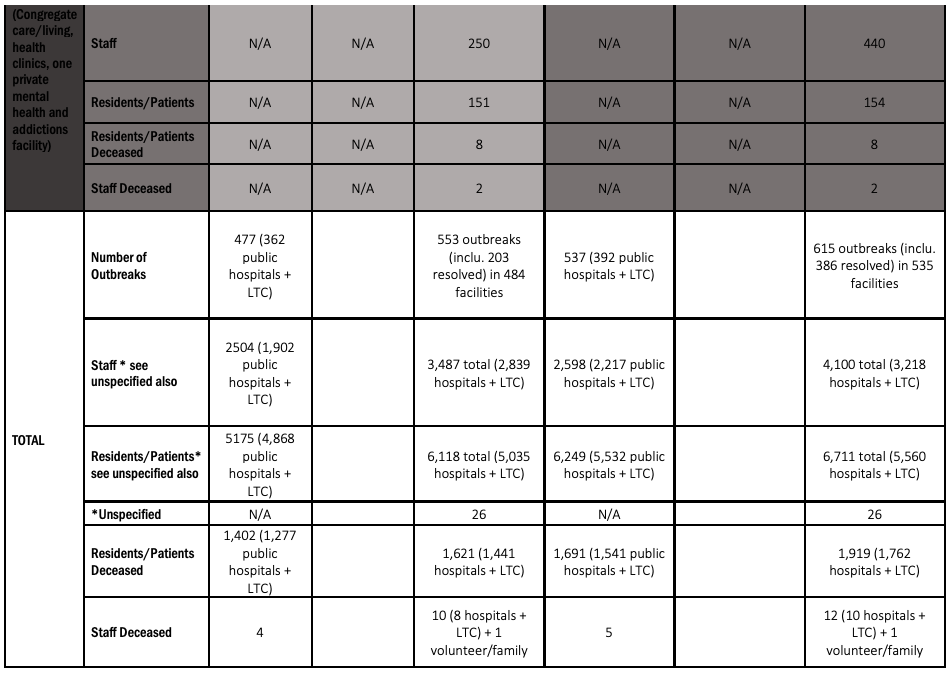
- The total number of people infected by COVID-19 in health and congregate care settings including staff and patients/residents is 11,337 as of June 2, up from 9,361 as of May 19. This total increased by 1,976 people or 21.1 percent in two weeks, a faster growth rate from the previous two-weeks when the increase was 18.6 percent.
- The percentage of the total number of Ontarians infected with COVID-19 that are health care workers has decreased for the first time since we began tracking in mid-March but the raw number of health care workers infected with COVID-19 continues to rise. By June 2, out of a total of 29,047 people confirmed to have been infected 4,797 or 16.5 percent were health care workers, according to Public Health Ontario. From May 19 to June 2 the total number of health care workers infected increased by 686 workers, an increase of 16.7 percent in two weeks. This rate of increase is down from the high of 67.7 percent in the month leading up to May 5 but is still very significant.
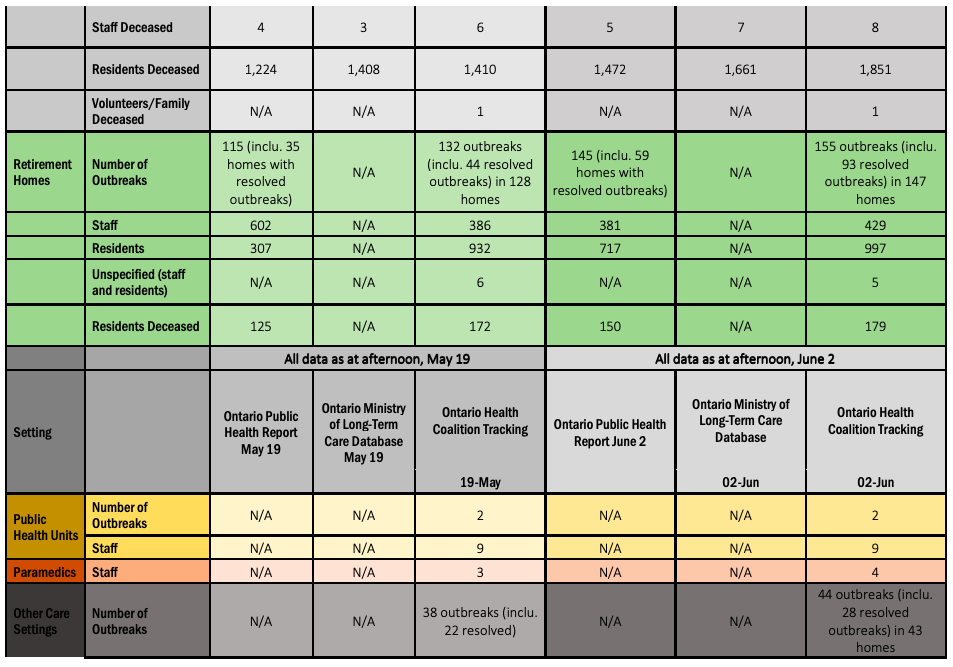
- The total number outbreaks in health care and congregate care settings that the Ontario Health Coalition found as of June 2 is 615 (including 386 resolved) in 535 facilities including hospitals, long-term care homes, retirement homes Public Health Units, clinics and other congregate care settings. As of May 19 we found 553 outbreaks (including 204 resolved) in 484 facilities. The number of outbreaks that are active across health care settings that we have found is now 229 compared to 349 two weeks prior (May 19), thus, the first significant decrease (though we may not have been able to find all outbreaks as there is less public reporting now than there was in April through to early May).
- The total number of patients/residents that have been infected by COVID-19 in health and congregate care settings has also increased. By June 2 we have tracked a total of 6,711 patients/residents who have contracted COVID-19 in health and congregate care settings. This is an increase of 593 patients/residents in two weeks (since May 19) or 9.7 percent. This is still unfortunately a significant increase, but down from the 23.6 percent increase we calculated between May 5 and May 19.
- Tragically, the death toll among patients, residents and staff in health and congregate care settings has also increased dramatically. The Ontario Health Coalition is deeply sorry to report that as of June 2, we found a total of 1,919 patients and residents deceased in outbreaks in health and congregate care settings, up from 1,621 deceased as at May 19. That increase amounts to a heartbreaking 298 residents and patients over two weeks or an increase of 18.4 percent.
- Chart 3 tracks the large outbreaks (more than 10 people infected with COVID-19) in health and congregate care settings. As at June 2, using this definition of large outbreaks we had found a cumulative total of 162 facilities with 201 outbreaks. Included in these numbers are 38 facilities in which the numbers of staff and patients/residents infected and the number of deaths had not changed since two weeks ago (May 19) and it also includes 51 outbreaks that are clearly declared resolved with no new outbreak.
Note about Methodology: In order to compile this list, we have tracked the daily updates from the 34 Public Health Units in Ontario, including the epidemiological details and outbreak reports where they are publicly available. We have searched each facility name to identify whether it is long-term care or a retirement home and to find details about the cases reported in the aggregate numbers by Public Health Units. We have tracked and compiled media reports of outbreaks with details from across Ontario that contain credible source information (for example, they cited the Public Health Unit, long-term care home administration or hospital administration). Local Public Health Units report in different ways with varying levels of detail. Some do not provide breakdowns of staff/patients/residents. Local Public Health Units usually post outbreak reports for public hospitals, long-term care and retirement homes. The provincial-level information from Public Health Ontario does not include retirement homes or other health care and congregate care/living settings. We have tried to capture everything we can about retirement homes and other health care settings in addition to hospitals (public and private) and long-term care homes using the methodology outlined here. We have not been able to catch up on shelters, group homes and all the various congregate care settings. For that we apologize and will try to capture as much as we can going forward. It is not clear why Public Health Ontario’s numbers for the outbreaks in long-term care and public hospitals are lower than ours. We have repeatedly checked ours for accuracy and we have provided information in the most transparent way possible. In addition, Public Health Units are reporting retirement home outbreaks separately and these numbers should be available to Public Health Ontario but Public Health Ontario does not report the aggregate numbers for retirement homes. Given the number of outbreaks in these private for-profit homes, it is important that the spread in them is also tracked and that they are subject to improved public health measures (and the support needed) to protect residents and staff. Overall, we have tracked every individual case and report in the most credible manner possible and have included sources for each report in the footnotes.